Healthcare
Hospitals, Clinics, and Healthcare Services
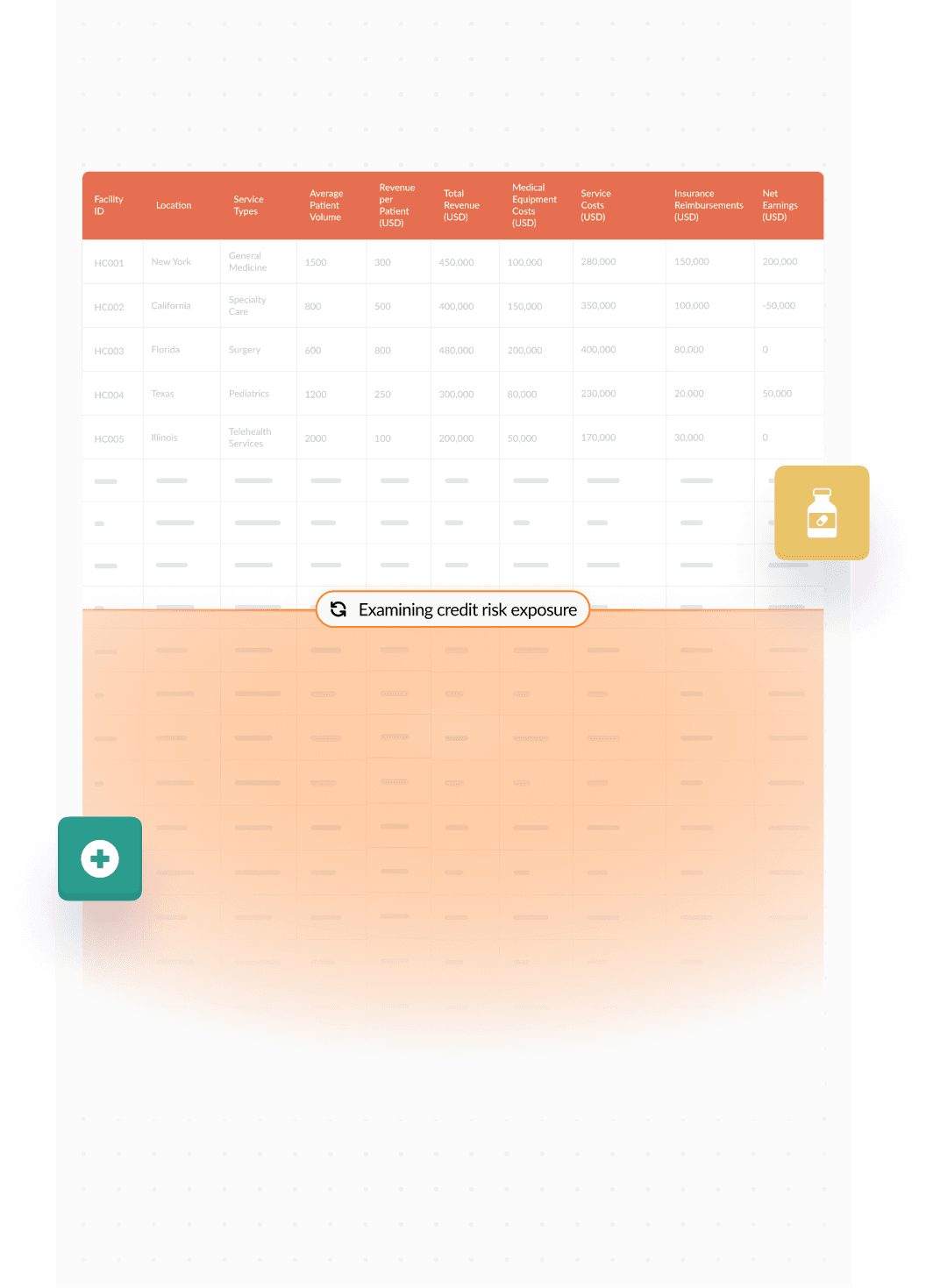
Financial & Capital Analytics
Hospital Revenue Cycle Management: Analyze patient flow from registration to billing and collections. Assess the impact of patient volume fluctuations, treatment mix, and insurance claim denials on cash flow and financial health
Clinic Performance Metrics: Evaluate financial performance metrics for outpatient clinics, including patient turnover rates and average revenue per patient. Focus on the economics of scale in operations and the financial impact of appointment no-shows
Pharmaceutical Sales Trends: Scrutinize revenue streams from pharmaceutical sales, considering the effect of patent expirations, generic competition, and pricing strategies on profitability
Healthcare Facility Optimization: Optimize portfolios by assessing the financial viability of healthcare facilities. Identify underperforming locations and potential for service expansion or reallocation based on community health needs
Medical Equipment Utilization: Balance the investment in medical technology with usage rates and maintenance costs to ensure optimal financial returns. Evaluate the lifecycle costs of high-value medical equipment
Procedure Demand Forecasting: Investigate trends in medical procedures driven by demographic changes and disease prevalence. Use this data to forecast demand for specific healthcare services and align resource allocation
Healthcare Consumer Behavior: Conduct deep dives into patient behavior, including preferences for telehealth services versus in-person visits. Analyze the financial implications of these trends on healthcare delivery models
Cost and Profitability Analysis: Develop financial models that detail the costs associated with different healthcare services. Model profitability by patient group, service line, or treatment type to guide pricing and investment decisions
Risk Adjustment Models: Create models that predict financial risk and resource needs based on patient demographics and health conditions. Use these models to adjust financial planning and ensure adequate resource allocation for high-risk populations
Funding Strategies for Healthcare Innovation: Identify the best mix of financing options to support investments in healthcare innovations, such as new medical procedures or digital health technologies
Financial Planning for Healthcare Systems: Develop financial strategies that support the complex needs of integrated healthcare systems, including capital investments for expansion and technology upgrades
Insurance Reimbursement Variance: Track variances between expected and actual insurance reimbursements. Analyze reasons for discrepancies and adjust billing processes to maximize revenue capture
Operational Cost Management: Monitor and manage variances in operational costs, such as staffing and supply chain expenditures. Use variance analysis to identify inefficiencies and implement cost-saving measures
Pandemic Impact Analysis: Assess the financial impact of pandemics on healthcare operations. Develop strategies to mitigate risks related to sudden changes in patient volumes and service demands
Technology Adoption Risks: Evaluate the financial risks associated with adopting new healthcare technologies. Develop risk mitigation strategies that address potential disruptions to existing workflows and patient care delivery
Healthcare Network Expansion: Analyze potential M&A opportunities to expand healthcare networks. Consider the financial and operational synergies of integrating new facilities or services
Specialty Practice Acquisitions: Evaluate the benefits and risks of acquiring specialty practices. Assess how these acquisitions can enhance service offerings and improve financial performance within broader healthcare systems
Business Intelligence
Compile patient admission rates, treatment outcomes, and healthcare provider efficiency to assess overall facility performance
Investigate the reasons for high readmission rates or patient dissatisfaction by analyzing treatment protocols, staffing patterns, and patient feedback
Use historical health data and demographic trends to predict future disease outbreaks or patient influx, helping to optimize resource allocation and readiness
Recommend changes in staffing levels, patient care strategies, or health monitoring programs based on predictive analytics to improve patient outcomes and operational efficiency
Integrate data from clinical trials, patient records, and real-time health monitoring to infer patterns that could lead to new treatment protocols and preventive health strategies
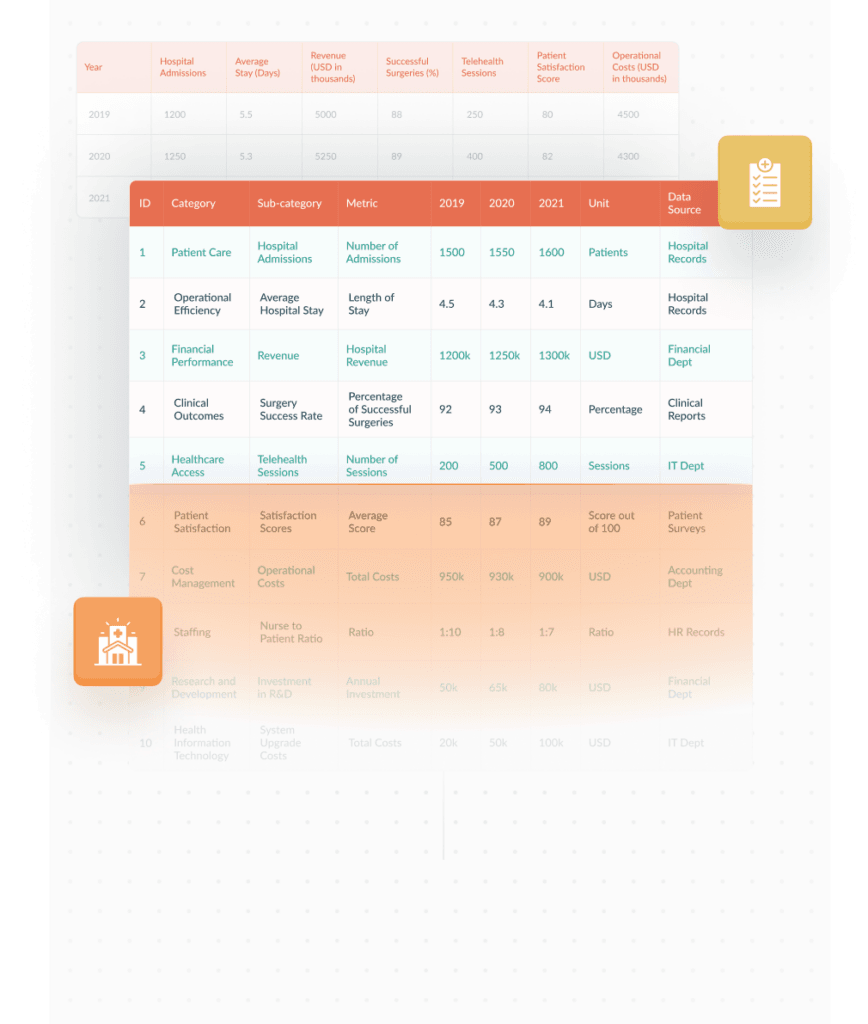
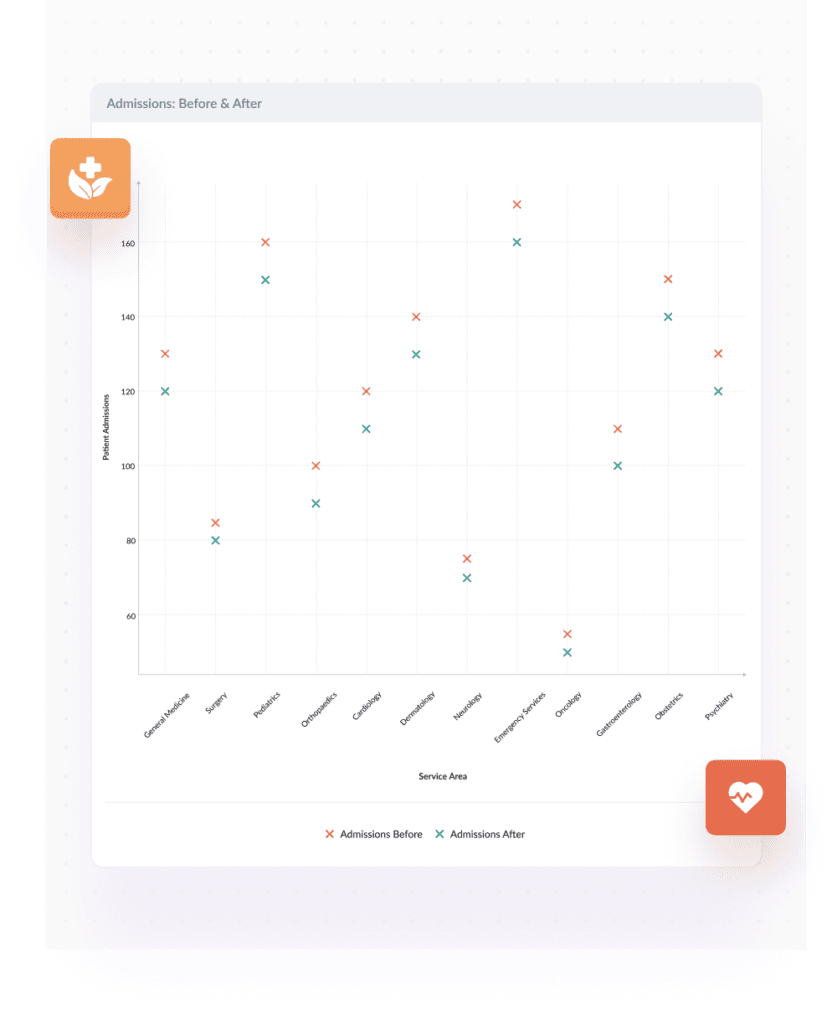
Streamlining
Examine all healthcare delivery processes, from patient intake to treatment and discharge. Identify bottlenecks such as lengthy administrative procedures or inadequate patient flow management
Implement electronic health records (EHRs), automated appointment scheduling systems, and patient monitoring technologies to reduce paperwork and enhance patient care coordination
Monitor metrics such as patient wait times, treatment outcomes, staff productivity, and patient satisfaction to evaluate service effectiveness and identify improvement areas
Merge administrative functions or centralize purchasing for medical supplies across facilities to reduce costs and streamline operations
Develop standardized treatment protocols, hygiene practices, and patient care procedures to ensure high-quality and consistent care delivery
Establish continuous feedback systems involving patients, medical staff, and administrative personnel to promptly address issues and innovate care practices
Review whether the implemented streamlining processes have improved care efficiency, patient outcomes, and cost management. Adjust policies and practices as needed based on these reviews